GUM DISEASE AND DIABETES
One in three humans has some form of gum disease.
Diabetes Mellitus is a disease which is caused by insulin deficiency and or resistance.
In ancient India, it was described as the disease with “honey urine”, because it was established that ants were attracted to the urine of the sufferer.
Diabetics fight a life time battle to control infections because of defective or compromised immunity that expresses itself in delayed responses at the cellular level.
In the last two decades, researchers have uncovered inextricable linkages between Gum disease and many other illnesses.
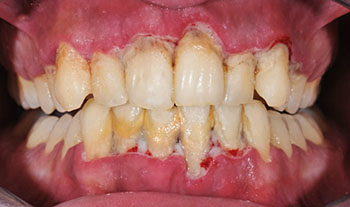
The bacteria that cause gum disease have been linked with as many disparate conditions as heart disease, diabetes, arthritis, Alzheimer’s, stroke and adverse pregnancy outcomes.
These bacteria chiefly P. Gingivalis, P. Intermedia and T Denticola join with other bacteria to synergistically cause a type of inflammation that over time, affects the immune system reactions in the body.
Diabetes and Periodontal Disease:
So serious is this link that Periodontitis is considered the sixth complication of diabetes alongside neuropathy and blindness. Diabetics are three times more likely to have advanced periodontal disease than the non-diabetic.
There is a two-way relationship between gum disease and diabetes that worsens both conditions.
Poor sugar control is found to lead to periodontitis, but the inflammatory response to periodontitis hinders the diabetics healing responses. How does this happen?
Because periodontitis causes inflammation it triggers immune responses in the whole body. The Diabetics defective immune response causes poor glycemic control which worsens the diabetic condition. When gum disease has set in, it worsens far more rapidly in a diabetic, with fulminating bone loss and massive shedding of teeth within a matter of a few years.
Apart from gum disease, certain other mouth conditions are common in diabetics; Xerostomia [ dry mouth, caused by lack of saliva], and Candidiasis or oral thrush.
What should diabetics do? The diabetic should control their sugar levels as finely as possible under the care of their physician. Preventive dentistry is essential.
The Diabetic must keep their mouth in tip top shape. It is essential to have bi-annual dental checkups with charting of the gums of the diabetic to identify bone loss, and to carry out scaling and polishing.
“The nonsurgical treatment of periodontitis improves the glycemic status and levels of glycated hemoglobin, and therefore proves the great importance of oral health in these patients,” José López-López, DDS, MD, PhD, professor, Department of Dentistry, University of Barcelona Dental School, Barcelona, Spain.
“The mouth reflects the body.”


